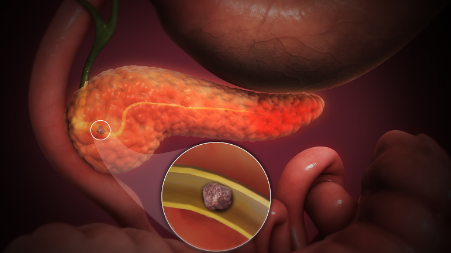
A sudden, sharp pain in the upper abdomen that does not seem to go away can be difficult to ignore, especially when it begins to interfere with daily activities. Many people initially mistake it for a minor digestive issue, which can delay timely medical care. In India, the rising number of such cases reflects changes in daily habits, diet, and alcohol consumption, making early awareness even more important.
These symptoms are often associated with pancreatic conditions, such as acute pancreatitis, where timely diagnosis is important. In such cases, appropriate treatment of pancreatic infection can support recovery and reduce complications. Identifying factors like alcohol use and lifestyle habits can help individuals take steps to protect their pancreatic health and seek timely care.
What Is Acute Pancreatitis?
Acute pancreatitis occurs when digestive enzymes become active within the pancreas instead of the intestine, leading to irritation and inflammation of pancreatic tissues. The condition can vary in severity, with some cases mild and others requiring closer medical supervision. Common signs often include persistent upper abdominal pain, nausea and vomiting, fever or discomfort after eating, and a reduced appetite. Recognising these symptoms early is important, as it supports timely medical evaluation and appropriate treatment for pancreatic infection.
How Alcohol Can Affect the Pancreas
Alcohol consumption can affect pancreatic health and may increase the risk of acute pancreatitis in some individuals. Regular or excessive intake can disrupt normal pancreatic function and contribute to inflammation. Biologically, alcohol may trigger premature activation of digestive enzymes in the pancreas rather than in the intestine, leading to irritation and inflammation of pancreatic cells. Over time, repeated exposure can also cause structural changes in pancreatic tissue, affecting its overall function.
Alcohol can contribute to pancreatitis by:
- Increasing enzyme activity within the pancreas.
- Causing narrowing or blockage in the pancreatic ducts.
- Leading to repeated irritation over time.
The risk is generally higher in individuals who consume alcohol frequently or in larger amounts. Repeated episodes may sometimes increase the likelihood of longer-term changes in pancreatic health.
Lifestyle Factors Behind Acute Pancreatitis
Lifestyle-related factors have become increasingly relevant in recent years. Changes in diet, reduced physical activity, and metabolic conditions have contributed to the rise in cases.
- Diet and Gallstones: A high-fat diet may increase the risk of gallstone formation. These stones can block the pancreatic duct, leading to inflammation.
- Obesity and Metabolic Health: Excess body weight is associated with higher levels of triglycerides and other metabolic changes. These factors can affect pancreatic function and increase the risk of acute episodes.
- Smoking and Inactivity: Smoking affects pancreatic health and may worsen inflammation. Limited physical activity further contributes to metabolic imbalance, which can influence disease progression.
These factors often develop gradually, making them less noticeable until symptoms appear.
Alcohol vs Lifestyle: Key Differences
Both alcohol and lifestyle factors play a role in acute pancreatitis, but their impact differs in how the condition develops. Alcohol often acts as a direct trigger and may lead to the sudden onset of symptoms.
In contrast, lifestyle-related factors increase risk gradually over time. These include frequent consumption of high-fat and fried foods, being overweight, low physical activity, smoking, and poorly managed conditions such as high triglyceride levels or diabetes.
Alcohol-related cases may present earlier in individuals with frequent consumption, while lifestyle-related cases are often linked to long-term dietary and metabolic patterns. In many situations, both factors coexist. For example, individuals with unhealthy dietary habits and regular alcohol intake may face a higher risk compared to those exposed to a single factor.
Why Is Acute Pancreatitis Increasing in India?
The rising number of cases in India reflects broader lifestyle and dietary changes across different populations. Shifts in eating patterns, including increased intake of processed and high-fat foods, have contributed to metabolic health concerns. At the same time, alcohol consumption patterns vary across regions and communities, and remain an important contributing factor.
Additionally, conditions such as obesity, diabetes, and high triglyceride levels are more prevalent today. These factors, together, create an environment in which pancreatic health may be more frequently affected.
Role of Early Diagnosis and Medical Care
Early diagnosis is important for managing acute pancreatitis. Identifying the cause helps guide treatment and prevents further complications.
Doctors may recommend:
- Blood tests to assess enzyme levels.
- Imaging methods such as ultrasound or CT scans.
- Clinical evaluation based on symptoms.
Timely treatment of pancreatic infection focuses on supporting recovery and addressing the underlying cause. Medical supervision also helps monitor the condition and reduce the risk of recurrence.
How to Reduce the Risk of Acute Pancreatitis?
Managing both alcohol-related and lifestyle-related risks can support pancreatic health and may help lower the likelihood of acute pancreatitis. Small, consistent changes can make a meaningful difference. Key preventive steps include:
- Limit or avoid alcohol to reduce pancreatic stress.
- Follow a balanced, low-fat diet.
- Stay physically active to maintain a healthy weight.
- Manage metabolic conditions such as diabetes or high triglycerides.
- Avoid smoking to reduce inflammation.
Regular check-ups can help detect early signs and provide guidance on managing these risks effectively.
Conclusion
Acute pancreatitis can be influenced by both alcohol use and lifestyle factors, each affecting pancreatic health in different ways. While alcohol may sometimes act as a trigger, lifestyle habits often increase risk gradually over time. In India, the combination of these factors has contributed to a rise in cases. Awareness, regular monitoring, and timely medical consultation can help manage potential risks. Seeking appropriate treatment for pancreatic infections when needed and following medical guidance may support healthier pancreatic function and overall well-being.